Why do our children self-harm and why aren’t we talking about it? Self-harm is one of the most misunderstood issues we face in working with young people and their mental health.
Kelly was in my Year 8 class. She was quiet, but not unusually so. A nice kid. One afternoon, it was screamingly hot, in the way only Perth in summer can be. She had her jumper on. I asked her to take it off. I was afraid she would pass out. She looked at me blankly. “Kel, it’s just too hot.” She quietly said she couldn’t. She just couldn’t.
After class, we had a chat and she showed me the burns on her arms, self-inflicted with a lighter. Scars that had been there for months and wounds that were only days old. I wish I could say it was my first experience with self-harm but it wasn’t. It is so awfully common.
Self-harm is one of the most misunderstood issues we face in working with young people and their mental health. It is often dismissed as attention-seeking and self-indulgent. For that reason, it is surrounded by an enormous amount of shame for both the child and those who love and care for them.
What is self-harm?
Psychologist, Bethany O’Regan says, “Usually when people talk about self-harm, they are talking about non-suicidal self-injury. That’s things like cutting, burning, deliberately breaking bones, hitting one’s head against walls etc. However, self-harm can also include less obvious behaviours that have a deliberate, detrimental effect on a person, like binge drinking, highly promiscuous behaviour, driving recklessly, etc.”

Why do young people self-harm?
There are lots of reasons why a person might self-harm. Often it goes hand in hand with an ongoing mental health problem such as depression or anxiety, eating disorders, OCD, bipolar, or psychosis. Generally, what happens is that someone is unwell and it will get to a point where they feel that they can’t manage their emotional pain, this often results in self-harm.
There is something primeval and instinctive about hurting your own body. A threat exists for the harmer. Usually, when a threat is identifiable we fight it or fly from it. In the case of depression or anxiety or other internal trauma, the only enemy to combat is the self. So, on some level, it makes sense to self-harm.
It is interesting to note that self-harm, such as head banging and hitting, is quite common in the disabled community, particularly among people who are non-verbal. It appears to be a way of dealing with emotions when there is no other way of expressing or controlling them. Many neurotypical people who self-harm have similar struggles. They are trying to reduce arousal levels and take back control of their overwhelming feelings.
Self-harmers have a lot of built-up negative emotions: pain or hurt or anger or frustration or self-loathing, and they try to relieve it in a physical way with self-harm. It gives them an external focus for internal trauma. The resulting wound also gives them a focus as they have to care for it. That self-care is something they are unable to achieve emotionally.
Other people engage in self-harm to simply feel something. They report feeling completely numb inside. The intensity of the negative emotions that they experience become so intense that they disassociate. When a person disassociates it is to protect themselves from trauma. However, it’s not a state that can be sustained. The numbness itself becomes the problem. Self-harming is a way of feeling something, anything, even if that something is pain.
There is scientific evidence to support the idea that self-harming does actually make some people feel better. We experience physical and emotional pain in the same part of the brain. When you stub your toes or jam your finger in a door you experience a shot of extreme pain, but if you wait a few seconds it lessens considerably all of a sudden. That happens because the brain releases pain killer endorphins to protect you. Those endorphins also soothe emotional pain. So, while self-harming can cause pain to begin with, once those endorphins kick in they can make a person in huge emotional distress feel better.
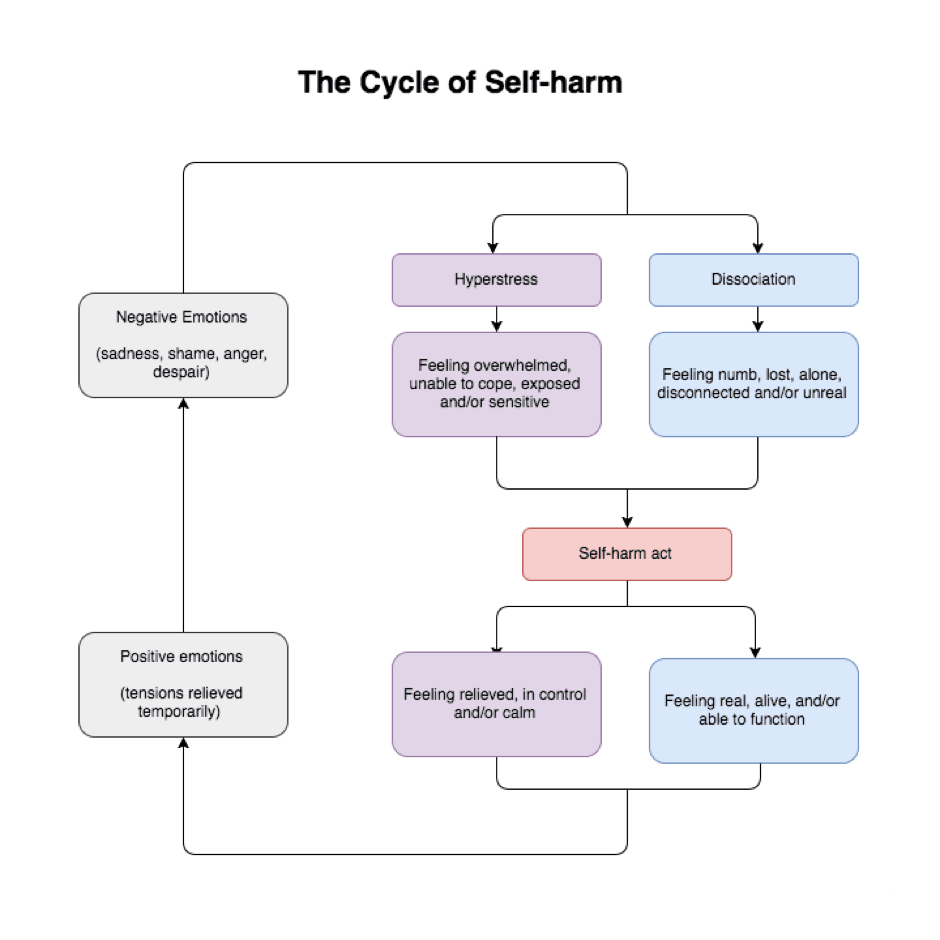
Whatever the reason, self-harm is a temporary fix because the initial positive effects pass. In their place, emotional pain builds again and the cycle repeats itself.
How many young people are self-harming?
The statistics are not very reliable because they are self-reported. There is a lot of shame around self-harm so the number of actual instances may be higher than reported. That said, The Australian National Epidemiological Study of Self-injury (ANESSI) reports:
- About 5% of 10 to 17-year-olds have deliberately injured themselves in the past year
- About 7% of 18 to 24-year-olds have deliberately injured themselves in the past year
- About 2.5% of 10 to 24-year-olds have deliberately injured themselves in the past four weeks
The youngest child Ms O’Regan has worked with was a 12-year-old girl.
Are self-harmers more likely to suicide?
By definition, when a person is self-harming, they are not trying to kill themselves. The objectives are far more complicated. However, there is always the risk of accidental death.
If a person who self-harms becomes even more despairing and their pain and illness escalate, then yes, they are at risk of suicide. Like self-harm, suicide presents as a logical answer to an existing problem. Our challenge is to be present enough that we see the warning signs and are able to offer other answers.
What about the theory that, ‘They’re just doing it for attention’?
They’re not. It would be extremely rare to self-harm for attention. Kids are often very secretive about it. Many will harm the soles of their feet, the groin area or the abdomen so that it is never discovered. People who self-harm are in need. They need help with the underlying problems. They need help to find different coping strategies. And they need a lot of understanding.
Why not follow Linda’s blog? You’ll receive useful information to help support your kids as they navigate their school years.
Australian Helplines
beyondblue aims to increase awareness of depression and anxiety and reduce stigma. Call 1300 22 4636, 24 hours / 7 days a week.
eheadspace provides mental health and wellbeing support, information and services to young people aged 12 to 25 years and their families. Call 1800 650 890.
Kids Helpline is Australia’s only free 24/7 confidential and private counseling service specifically for children and young people aged 5 to 25. Call 1800 55 1800.
Lifeline provides 24-hour crisis counseling, support groups and suicide prevention services. Call 13 11 14.






